Knee Replacement
for Diabetic Patients
What changes, what doesn't, and what every diabetic patient needs to know before proceeding.
Key Takeaways
- Diabetes is not a contraindication for knee replacement. Thousands of diabetic patients undergo successful joint replacement every year.
- Your HbA1c level matters. I prefer it below 8% before scheduling surgery, and ideally closer to 7%.
- The main risks to manage are wound healing and surgical site infection, both of which improve significantly with good perioperative sugar control.
- Preparation is everything. Optimising your diabetes before surgery is not a delay. It is part of the surgery itself.
- Long-term outcomes for diabetic patients with well-controlled sugars are comparable to non-diabetic patients.
A few weeks ago, a retired school teacher from Thalassery sat across from me in my outpatient clinic at Aster MIMS Kannur. Her knee X-rays were straightforward: advanced osteoarthritis, bone on bone, Grade IV changes in both the medial and patellofemoral compartments. She had been limping for three years. She needed a knee replacement. She knew it. Her family knew it.
But the first thing she said was not about the knee.
"Doctor, enikku sugar undu. Ippo surgery cheyyaan pattuo?"
("Doctor, I have diabetes. Can I still have surgery?")
I hear some version of this question almost every day. It comes from patients in their sixties who have been living with Type 2 diabetes for a decade or more. It comes from Gulf returnees who have managed their sugar "on and off" for years. It comes from anxious sons and daughters who read somewhere online that diabetic patients should not undergo major surgery.
So let me answer this directly, the same way I answer it in clinic.
Diabetes does not disqualify you from knee replacement. But it does change how we prepare, how we manage the perioperative period, and what we watch for during recovery. The surgery itself is not fundamentally different. The care around it is.
Why does diabetes come up so often in knee replacement discussions?
There is a simple reason: the two conditions overlap enormously in the same population. Type 2 diabetes and knee osteoarthritis both become more common with age, with higher body weight, and with sedentary lifestyles. In Kerala, where diabetes prevalence is among the highest in India, I see this overlap in my practice every single week. A large number of my patients at Aster MIMS Kannur, whether from Kannur itself or referred from Kasaragod, Wayanad, or Payyannur, have diabetes as a co-existing condition.
The concern is not unfounded. Diabetes does affect how the body heals, how it fights infection, and how it responds to the stress of surgery. But these are risks to be managed, not reasons to refuse treatment and leave someone in pain for years.
What HbA1c level do I need before knee replacement?
HbA1c is the blood test that tells us how your sugar has been controlled over the past two to three months. It is a far more useful number than a single fasting sugar reading, because it shows the trend, not just a snapshot.
Here is how I think about it in practice:
- HbA1c below 7.5%: Ideal. We proceed with confidence.
- HbA1c between 7.5% and 8%: Acceptable. We proceed with close monitoring.
- HbA1c between 8% and 9%: I ask you to work with your physician or diabetologist first. We postpone surgery by a few weeks, not indefinitely. Once we see improvement, we schedule.
- HbA1c above 9%: I will not schedule elective surgery. The infection risk and wound healing problems become too significant. We need a focused effort to bring your diabetes under better control, and then we revisit.
Let me be honest about this: postponing surgery to optimise your diabetes is not me being overcautious. It is me protecting your result. A knee replacement that gets infected because of poor sugar control is a far worse outcome than waiting eight more weeks.
I understand that for a patient who has been suffering for years, being told to "wait a little longer" is frustrating. But I have this conversation honestly, and most patients, once they understand the reasoning, are willing to put in the work.
How do we prepare a diabetic patient for knee replacement?
Preparation for a diabetic patient is more involved than for a non-diabetic patient, but none of it is complicated. It simply requires coordination between your surgeon, your physician, your anaesthetist, and you.
Step 1: Baseline Assessment
We check your HbA1c, fasting and postprandial sugar levels, kidney function, urine microalbumin, and a cardiac evaluation. If you have been diabetic for more than ten years, I also want to know about any peripheral neuropathy, because this can affect how you perceive pain and participate in rehabilitation.
Step 2: Sugar Optimisation
If your HbA1c needs improvement, we work with your diabetologist to adjust your medications. For some patients this means adding or changing oral drugs. For others it means starting insulin temporarily. This phase can take four to eight weeks. I use this time productively: we begin physiotherapy to strengthen the muscles around your knee before surgery, which makes post-operative recovery easier.
Step 3: Medication Adjustments Before Surgery
Metformin is usually stopped 24 to 48 hours before surgery to reduce the rare risk of lactic acidosis under anaesthesia. SGLT2 inhibitors (medicines like dapagliflozin or empagliflozin) are stopped a few days before because of the risk of euglycaemic ketoacidosis. Insulin regimens are modified on the morning of surgery. Your anaesthetist will give you a clear, personalised plan. The message I give every patient: do not stop any medicine on your own without checking with us first.
Step 4: Infection Prevention Protocol
For diabetic patients, I am particularly meticulous about infection prevention. This includes screening for urinary tract infections and dental infections before surgery (both common in diabetic patients and both potential sources of bacteria that can reach the new joint), nasal decolonisation with mupirocin, and perioperative antibiotics timed precisely with the first incision.
Does the surgery itself change for a diabetic patient?
The operation, the actual process of replacing the arthritic joint surfaces with an implant, is the same. I use the same implants, the same surgical approach, and the same precision whether a patient is diabetic or not.
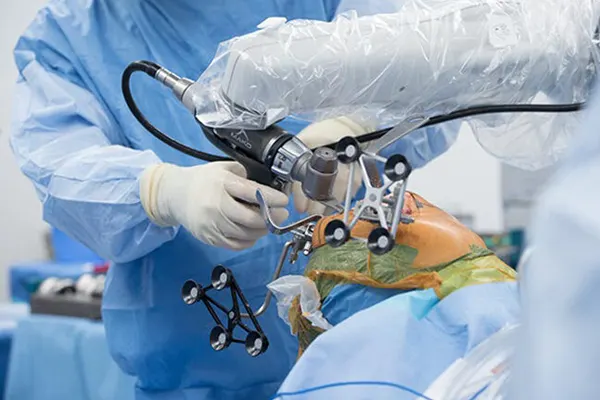
When I use the CORI robotic-assisted system for total knee replacement, the technology does not differentiate between a diabetic and a non-diabetic knee. What it does, for every patient, is create a real-time 3D map of the bone surface and guide my cuts with sub-millimetre accuracy. For a diabetic patient, this precision has a secondary benefit: more accurate bone preparation means less unnecessary soft tissue handling, which is a small but welcome advantage when you are already asking the body to heal under slightly less-than-ideal conditions.
What about surgical time?
I do not rush any surgery, but I am mindful that prolonged operating time increases infection risk for all patients, and slightly more so for diabetic patients. Efficient surgery with minimal tissue exposure is one of the practical ways we reduce risk. This is a matter of surgical planning and discipline, not speed.
The real concerns: wound healing and infection
I will not minimise this. The two areas where diabetes genuinely makes a difference in knee replacement are wound healing and infection risk. Let me explain both.
Wound Healing
High blood sugar impairs the function of white blood cells, slows collagen synthesis, and reduces blood flow to small vessels at the wound edges. The result is that a diabetic patient with poorly controlled sugars heals more slowly, and the wound is more vulnerable in the critical first two weeks after surgery.
The good news is that this risk drops substantially when blood sugar is well controlled perioperatively. During the hospital stay, we monitor sugar levels multiple times a day and use a sliding scale insulin protocol to keep levels in the target range. This is standard care for every diabetic patient undergoing surgery at Aster MIMS.
Surgical Site Infection
Published data consistently shows that diabetic patients have a higher rate of periprosthetic joint infection compared to non-diabetic patients. The numbers vary across studies, but the absolute risk remains low: we are talking about moving from roughly 1% to perhaps 2–3% in patients with well-controlled diabetes.
For patients with poorly controlled diabetes (HbA1c above 8%), the risk climbs higher. This is precisely why I insist on optimisation before surgery. It is not a bureaucratic hurdle. It is the single most impactful thing we can do to protect you from the most serious complication of joint replacement.
A periprosthetic infection after knee replacement is not like a skin infection you treat with a course of antibiotics. It can mean re-operation, prolonged antibiotics, and in the worst cases, removal of the implant. Preventing it is always better than treating it.
Recovery and rehabilitation: what is different?
For most diabetic patients with reasonable sugar control, the rehabilitation timeline is very close to what I prescribe for non-diabetic patients. You will be standing and taking steps with a walker on the first day after surgery. Knee bending exercises begin immediately. Most patients are walking independently within three to four weeks and resuming their normal household activities by six to eight weeks.
What I watch more carefully in diabetic patients:
- Wound checks: I see diabetic patients slightly more frequently in the first two weeks, specifically to inspect the wound for any early signs of delayed healing or infection.
- Blood sugar monitoring: Surgery itself causes a stress response that can spike sugar levels for several days. We manage this actively during the hospital stay and give you clear guidance for the first two weeks at home.
- Neuropathy awareness: If you have diabetic neuropathy in your feet, your balance and proprioception may be affected. I factor this into your physiotherapy programme and sometimes recommend a longer period of walking with support.
"Will I be able to sit on the floor?"
Many of my patients in North Kerala ask whether they will be able to sit on the floor after knee replacement. This question comes up regardless of diabetes, but I mention it here because diabetic patients sometimes have stiffer joints to begin with.
My honest answer: deep floor sitting (like sitting cross-legged for extended periods) is not a goal I set after knee replacement. Sitting on a low stool or chair, getting on and off the floor with support, using a western commode instead of an Indian-style toilet. These are practical adaptations that protect the implant and work perfectly well for daily life.
What about long-term outcomes?
This is the question that matters most, and the answer is reassuring. Multiple large studies, including registry data from thousands of patients, show that the long-term survival of knee implants in diabetic patients with controlled sugars is comparable to non-diabetic patients. The implants last just as long. Pain relief is just as good. Functional improvement is just as significant.
Where outcomes diverge is in the subset of patients with uncontrolled diabetes, especially those with HbA1c persistently above 8% and those with significant diabetic complications like nephropathy or peripheral vascular disease. For these patients, the conversation is more nuanced, and it is one I have honestly in clinic, weighing the benefits of pain relief against the higher perioperative risks.
But for the vast majority of diabetic patients I see, patients with Type 2 diabetes managed on oral medications or insulin with an HbA1c in a reasonable range, knee replacement is a safe and effective procedure that reliably restores mobility and quality of life.
For patients returning to the Gulf after surgery
A significant number of my patients at Aster MIMS Kannur are NRIs working in the Gulf, particularly in the UAE, Oman, and Saudi Arabia. Many of them developed both their diabetes and their knee arthritis during years of relatively sedentary work and dietary changes abroad.
One practical advantage of having your surgery within the Aster DM Healthcare network is continuity. Aster has hospitals and clinics across the GCC. If you have your knee replacement with me in Kannur, your follow-up appointments, physiotherapy reviews, and any concerns that arise after you return to the Gulf can all be managed within the same network. I coordinate with the team there, share your records, and ensure nothing falls through the gap that distance sometimes creates.
For a diabetic patient, this continuity matters even more, because your sugar management needs to continue seamlessly after you travel back.
A Final Word
If you have diabetes and your knee is limiting your life, do not assume surgery is off the table. It almost certainly is not. What it does require is a little more preparation, a little more coordination, and an honest conversation about where your sugar levels stand today and where they need to be.
Come in with your X-rays, your latest HbA1c report, and your questions. That is what the consultation is for.
Frequently Asked Questions
You can, but not until we bring them under better control. I typically want an HbA1c below 8% before scheduling surgery, and ideally closer to 7%. This is not about denying you treatment. It is about making the surgery safer and the recovery smoother. I will work with your physician or diabetologist to get you there.
Most orthopaedic guidelines recommend an HbA1c below 8% for elective joint replacement. I prefer to aim for below 7.5% where possible. If your levels are between 8% and 9%, we do not cancel your plans. We postpone, optimise, and then proceed. If your HbA1c is above 9%, we need a more serious conversation with your diabetes team first.
It can. Poorly controlled blood sugar slows down the body's natural healing process and makes the wound more vulnerable to infection. However, if your sugar levels are well managed before and after surgery, wound healing proceeds normally for most patients. The perioperative period, the two to three weeks around surgery, is where tight sugar control matters most.
Robotic-assisted surgery using the CORI system is not diabetes-specific, but the precision it offers benefits every patient, including those with diabetes. More accurate bone cuts mean better implant fit, which may reduce soft tissue stress and contribute to smoother early recovery. For a diabetic patient, anything that reduces unnecessary tissue handling is a welcome advantage.
Some medicines need adjustment. Metformin is typically stopped 24 to 48 hours before surgery. Insulin doses are modified on the morning of the procedure. SGLT2 inhibitors are usually paused a few days before. Your anaesthetist and I will give you specific instructions based on what you are taking. Do not stop anything on your own without asking.
Yes, the data on this is clear. Diabetic patients have a modestly higher risk of surgical site infection after knee replacement. But "higher risk" does not mean "high risk." With proper sugar control, antibiotic protocols, and careful surgical technique, the vast majority of my diabetic patients heal without any infection. The risk is manageable, not prohibitive.
For most diabetic patients with reasonably controlled sugars, the recovery timeline is very similar to non-diabetic patients. You will be walking with support on day one, bending the knee progressively over the first few weeks, and returning to most daily activities by six to eight weeks. What I watch more carefully in diabetic patients is wound healing in the first two weeks and blood sugar control during the hospital stay.
Absolutely. Aster MIMS Kannur is part of the Aster DM Healthcare network, which has hospitals and clinics across the UAE, Oman, and other Gulf countries. Many of my patients are NRIs who fly in for surgery, recover here for two to three weeks, and then continue their follow-up at an Aster facility closer to where they live. We plan for this from the start.