Robotic Knee Replacement
in Kannur
What patients need to know before surgery — from how the CORI system works to what recovery actually looks like.
Key Takeaways
- The robot does not perform your surgery. Your surgeon does — with robotic precision assistance from the CORI system.
- No CT scan is needed before surgery. The CORI system maps your bone anatomy in real time on the operating table.
- Most patients walk with support within 24 hours and go home by Day 3–5.
- This technology is now available right here in Kannur at Aster MIMS — no metro city travel needed.
Almost every week in my outpatient clinic at Aster MIMS Kannur, someone walks in with an X-ray in hand, a stiff knee, and a question that goes something like this:
"Doctor, I've heard about robotic knee replacement. Is it something I should consider?"
It is a fair question. Robotic-assisted surgery has changed how we plan and perform total knee replacements, and it is now available right here in Kannur. But there is also a good deal of confusion around it. Patients hear about "robots doing surgery" and picture something out of a science fiction film. Others assume it is simply a marketing label for the same old procedure. Neither is true.
This post is my attempt to give you a clear, honest account of what robotic knee replacement involves, who it helps, and what you should realistically expect if you are considering it in North Kerala.
What exactly does "robotic" mean in knee replacement?
Let me start by clearing up the biggest misconception. The robot does not perform your surgery. I do. The robotic system is a precision tool that I control during the operation, guided by a surgical plan built around your individual anatomy.
At Aster MIMS Kannur, I use the CORI Surgical System by Smith+Nephew. One of the things that sets CORI apart from older robotic platforms is that it does not require a preoperative CT scan. Instead, the system builds a three-dimensional model of your knee in real time, right there on the operating table. I map the surface of your bone at the start of the procedure using a handheld probe, and the CORI software constructs a personalised 3D plan from that data.
No CT Scan. No Extra Radiation.
This means no extra radiation exposure, no additional hospital visit for a CT scan, and no delay between imaging and surgery. Your standard X-rays and the intraoperative bone mapping are all the system needs.
Millimetre-Level Precision
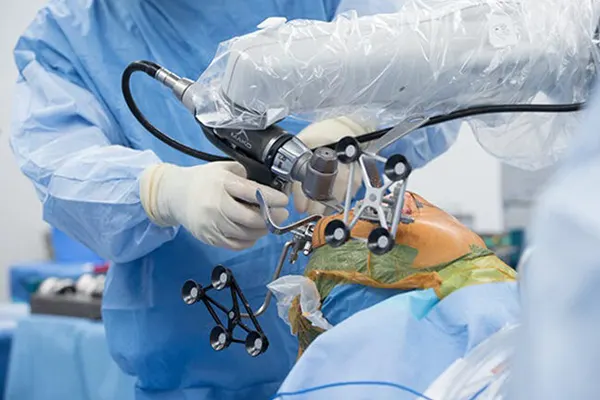
Once the plan is set, I use a handheld robotic burr to prepare the bone surfaces for the implant. The system provides continuous real-time feedback on my screen and controls the burr's speed and exposure, keeping me within the planned boundaries. If I approach the edge of the safe zone, the burr slows down and stops automatically. This gives me millimetre-level precision in implant positioning while I remain in full control of the instrument at all times.
Think of it this way: a skilled carpenter can cut wood freehand. But give that same carpenter a digitally guided tool that adjusts itself to the material, and the result is more consistent. The experience of the surgeon still matters enormously. The technology simply makes that experience more reproducible.
Why does this precision matter for your knee?
A total knee replacement is, at its core, a problem of alignment and balance. The artificial joint needs to sit at the correct angle on your bone, and the soft tissues around it need to be balanced so the knee feels stable through its full range of motion. Small errors in bone cuts — even two or three degrees of tilt — can affect how the implant loads over time. This can lead to uneven wear, persistent stiffness, or a knee that never quite feels "natural."
Robotic assistance reduces the margin of error in these cuts. Published data from multiple centres shows that robotic-assisted knee replacements achieve more consistent implant positioning compared to conventional manual techniques. For patients, this translates into a few practical benefits:
- Better early recovery, with many patients reporting less pain in the first few weeks.
- A more natural-feeling knee, because the implant alignment respects your native anatomy more closely.
- Potentially improved long-term implant survival, though the long-term data is still maturing.
I want to be careful here. Conventional knee replacement, done well, remains an excellent operation. I have performed hundreds of manual knee replacements with very good outcomes. Robotic assistance does not turn a bad surgeon into a good one. What it does is tighten the consistency of results, especially in complex or unusual knee geometries where manual planning has its limitations.
Who is a good candidate for robotic knee replacement?
Most patients who are candidates for a standard total knee replacement are also candidates for the robotic-assisted version. This includes people with:
- Advanced osteoarthritis of the knee that has not responded to medication, physiotherapy, or injections.
- Significant pain and functional limitation affecting daily activities like walking, climbing stairs, or getting up from a chair.
- Deformities such as bow legs or knock knees that make precise alignment especially important.
Where robotic planning is particularly valuable
Patients with extra-articular deformity (where the bowing originates from the thigh bone or shin bone rather than the joint itself), prior fractures around the knee, or retained hardware from old surgeries benefit considerably from the precision that the CORI system provides. In these complex cases, the intraoperative 3D mapping captures the actual state of your bone surfaces in a way that conventional jig-based instruments sometimes cannot account for.
That said, robotic knee replacement is not a magic solution for everyone. If your pain is primarily coming from a cause other than arthritis — referred pain from the hip or spine, for instance — replacing the knee will not solve the problem regardless of how precisely it is done. A thorough clinical evaluation remains the starting point.
What should you expect before surgery?
If we decide together that robotic knee replacement is right for you, the process at Aster MIMS Kannur typically follows these steps:
Initial consultation and workup
I examine your knee, review your X-rays, and discuss your symptoms, expectations, and medical history. If you have diabetes, hypertension, or cardiac issues, we coordinate with the relevant specialists to optimise your health before surgery. This is particularly important for our patients returning from the Gulf, many of whom have been managing these conditions with limited follow-up.
No CT scan required
Unlike some other robotic platforms, the CORI system does not need a preoperative CT scan. This means fewer hospital visits before surgery, no additional radiation, and a simpler preparation process overall.
Pre-anaesthetic assessment
Our anaesthesia team evaluates your fitness for surgery and discusses pain management options, including regional nerve blocks that significantly reduce post-operative discomfort.
Day of surgery
The procedure itself takes roughly 60 to 90 minutes. Most patients receive spinal anaesthesia (you are awake but feel nothing below the waist). You will not interact with the robotic arm during surgery.
Recovery: what is realistic?
I believe in being straightforward about recovery because I think unrealistic expectations cause more dissatisfaction after knee replacement than any surgical complication.
The first two weeks
These are the hardest. Your knee will be swollen. Walking with a walker or crutches is expected. Physiotherapy begins on the first or second day after surgery, initially focusing on gentle bending exercises and safe mobilisation.
By four to six weeks
Most patients are walking without a walker, managing stairs with some support, and returning to light household activities. Pain levels are usually manageable with simple oral medications by this point.
By three months
The majority of patients are walking independently, driving (if the operated knee is the left one, often sooner), and resuming most of their daily routine.
Full recovery: six to twelve months
This is the point at which the knee feels like a settled, reliable part of your body rather than something you are constantly aware of. The knee continues to improve in terms of stiffness and confidence well beyond the three-month mark.
"Will I be able to sit on the floor?"
One question I get asked frequently here in Kerala. Modern implant designs allow a good degree of deep flexion, and many of my patients do return to sitting cross-legged or on low seating.
But I counsel patients honestly: floor-level activities place higher stresses on the implant, and a chair-height lifestyle is better for the longevity of your new knee. The answer depends on your flexibility, your body habitus, and how your knee responds to rehabilitation. This is a conversation I have with every patient individually.
Why consider having this done in Kannur?
There was a time when patients from Kannur and the wider North Malabar region had to travel to Kochi, Bangalore, or Chennai for advanced joint replacement surgery. That is no longer the case.
At Aster MIMS Kannur, we have the infrastructure, the implant inventory, and the trained surgical and rehabilitation team to offer robotic-assisted knee replacement at a standard comparable to any major metro centre. For patients and their families, this means the considerable advantage of recovering close to home, with your support system around you, and with easy access to follow-up appointments without the cost and inconvenience of long-distance travel.
For NRI Patients from the Gulf
For our NRI patients visiting from the Gulf, the Aster brand is already familiar from its network of hospitals across the GCC. Having your surgery and initial recovery at Aster MIMS Kannur means continuity of care: if you need any follow-up after returning to Dubai, Abu Dhabi, or Muscat, your records are accessible within the Aster network. This seamless continuity gives Gulf-based Keralites the confidence to plan their surgery during a visit home, providing them with real peace of mind.
Patients from Thalassery, Kasaragod, Wayanad, Payyannur, and the wider North Kerala region can reach Aster MIMS Kannur within an hour or two — and stay close to family throughout their recovery.
A Final Word
Technology is only as good as the hands and the judgement behind it. I trained in joint replacement at PGI Chandigarh, and I continue to operate on a high volume of knee and hip replacements every year. The CORI system is a tool I have added to that foundation, not a replacement for it.
If you have been living with knee pain that limits your walking, disturbs your sleep, or stops you from doing the things that matter to you, it is worth having a conversation about your options.
You do not need to arrive at my clinic with a decision already made. Come with your X-rays, your questions, and your doubts. That is what the consultation is for.
Frequently Asked Questions
No. The CORI Surgical System is a precision tool that I control throughout the procedure. I hold the handheld robotic burr, make all surgical decisions, and guide every step of the operation. The system provides real-time feedback and boundary control to enhance accuracy, but the surgeon remains in charge at all times.
Not with the CORI system. Unlike some older robotic platforms that require a preoperative CT scan, CORI builds a three-dimensional model of your knee intraoperatively using bone surface mapping. This means no extra radiation, no additional hospital visit, and a simpler preparation process.
Yes. I perform CORI robotic-assisted knee replacements at Aster MIMS Kannur. Patients from Kannur, Thalassery, Kasaragod, Wayanad, and the wider North Malabar region no longer need to travel to Kochi or Bangalore for this procedure.
The procedure typically takes 60 to 90 minutes, comparable to a conventional knee replacement. The intraoperative bone mapping adds only a few minutes to the overall surgical time.
Most patients walk with support on the first or second day. By four to six weeks, most are walking independently and managing stairs. Full recovery, where the knee feels settled and natural, generally takes six to twelve months.
Modern implant designs allow significant knee bending, and many patients do return to sitting cross-legged. However, floor-level activities place higher stress on the implant over time. I discuss this honestly with each patient based on their individual flexibility, body habitus, and rehabilitation progress.
The cost is modestly higher due to the technology involved, but the difference is not prohibitive. I encourage patients to discuss the specifics during consultation, as costs can vary based on the implant chosen and your insurance coverage.
Absolutely. Many of my patients are Gulf-based Keralites who plan their surgery during a visit home. The Aster network's presence across the GCC means your records are accessible for any follow-up needed after you return to Dubai, Abu Dhabi, Muscat, or elsewhere in the Gulf.

How the CORI system delivers sub-millimetre precision for your knee replacement.
Day-by-day recovery guide covering pain, walking, home setup, and when to call your surgeon.
Recovery guides, procedure explainers, and evidence-based answers from Dr. Vishnu Baburaj.
Continue Reading
Robotic Knee Replacement at Aster MIMS Kannur
Your First Week After Total Knee Replacement
Browse All Patient Guides
At Aster MIMS Kannur, we bring robotic-assisted knee replacement to North Kerala — so you can recover where you belong.
"Your knee pain has already taken enough of your life.
Your Knee Deserves Precision.
You Deserve It Close to Home.
Let's get it back."