Key Takeaways
- You will stand and walk with a walker on Day 1 — this is modern recovery, not recklessness.
- Days 2–3 are the hardest — take your pain medications on time. Do not try to tough it out.
- Most patients go home by Day 3–4. Your own bed, your own food — these are powerful medicines.
- By the end of Week 1, the worst is behind you. You will feel the turning point.
If you've been putting off knee replacement surgery because you're afraid of "what happens after", this post is for you.
At Aster MIMS Kannur, I frequently meet patients who all say the same thing:
"Doctor, surgery okke cheyyaam. But after that? I've heard the first week is terrible."
I understand. You've heard the stories. Someone's neighbour's cousin apparently "couldn't even move for a month." Someone on WhatsApp said the pain is "worse than the knee pain itself." And now you're terrified.
Let me tell you the truth, not the WhatsApp version, but the version I share with my own family.
The first week after a Total Knee Replacement is challenging. But it is not terrible. And it is completely manageable once you know what to expect.
That is what this guide is for. Day by day. Just the honest truth from someone who has managed thousands of these recoveries, from my training days at PGIMER Chandigarh to my practice here in Kannur.
Day 0 — The Day of Surgery
"Wait, I Can Already Move It?"This surprises almost everyone.
Within hours of your surgery, the physiotherapy team will visit you. Yes, the same day. They will ask you to gently bend and straighten your new knee while you are still in bed.
What you'll feel
Surprisingly less pain than you expect. We use a combination of advanced nerve blocks and medications that keep you very comfortable in the first 12–24 hours. You will feel a heavy, tight sensation around the knee, like someone has wrapped a thick bandage very firmly. That is normal.
What you need to do
Wiggle your toes and pump your ankles up and down every hour. This is not optional. It keeps the blood flowing and prevents clots. Don't panic if the knee looks swollen. It will be. That is your body's natural healing response. Rest, but don't lie frozen like a statue. Small movements are your best friend right now.
Day 1
"I'm Standing Already?"This is the big day. You will stand up, with support, and possibly take a few steps with a walker.
I know what you're thinking. "One day after surgery and I'm walking?" Yes. This is modern knee replacement recovery. We don't believe in keeping you bedridden for days. Early movement is the single most important thing for a good result.
What you'll feel
Some pain when you first put weight on the leg. It is a sharp, uncomfortable pressure, but not the "unbearable agony" you've been warned about. On a scale of 1 to 10, most of my patients rate it between 4 and 6. Manageable with medication.
What you need to do
Trust the walker. It is carrying most of your weight. You are not going to fall. Take small steps — nobody is asking you to walk to Payyambalam Beach. Just three to four steps beside your bed is a victory. Do the exercises the physiotherapist shows you — gentle knee bending, straight leg raises. Even five repetitions matter.
Days 2–3
"Okay, This is the Hard Part"I won't lie to you. For most patients, days two and three are the toughest part of the first week.
The initial nerve block starts wearing off. The knee swells more. You feel stiff. The excitement of "I survived surgery" fades, and reality sets in.
What you'll feel
Increased pain and stiffness, especially in the morning or after you've been resting for a while. Sleep will be disturbed — finding a comfortable position is frustrating. You might feel low, irritable, or emotional. This is completely normal. Your body is healing from a major event.
What you need to do
- Take your pain medications on time. Do not try to "tough it out." Pain that is not managed properly will slow down your recovery because you won't be able to do your exercises.
- Ice the knee for 15 to 20 minutes, several times a day.
- Keep doing your exercises even though you don't feel like it. This is where recovery is won or lost. Patients who push through the discomfort on days two and three consistently recover faster.
- Walk to the bathroom with the walker. Walk in the hospital corridor if your doctor clears you. Every step counts.
Days 3–4 — Going Home
For Most PatientsAt Aster MIMS, most of our knee replacement patients go home by day three or four. Some of you reading this might be surprised: "So soon?" Think about it. Your own bed, your own food, your own bathroom. These are powerful medicines. Patients recover faster at home.
Before you leave, we make sure you can walk safely with a walker, get in and out of bed on your own, use the bathroom independently, and that your pain is controlled with oral medications. You and your family will understand the exercise routine and warning signs before discharge.
Home Setup — Do This BEFORE Surgery
- Keep a sturdy chair with armrests ready. Avoid low seats, low cots, and the floor. No sitting cross-legged for now.
- If you have an Indian-style toilet, arrange a commode chair or portable Western seat attachment — this is non-negotiable.
- Remove loose rugs, mats, and anything you might trip over. Get anti-slip mats if you have slippery tiles.
- Keep your medications, water bottle, phone, and TV remote within arm's reach.
Days 5–7
"I Think I Can Do This"By the end of the first week, you turn a corner. The worst of the swelling starts to reduce. Pain is noticeably less than it was on day two or three. You are walking to the kitchen, to the bathroom, maybe even to the veranda to watch the evening light over the coconut trees.
What you'll feel
You will feel more confident. Your knee still feels tight and stiff. It won't bend fully yet, and that is perfectly okay. Full bending takes weeks, not days. You can feel it getting a little easier each day.
What you need to do
- Continue your exercises religiously. Do them two to three times a day. Consistency beats intensity.
- Walk a little more each day. Inside the house is fine.
- Keep the leg elevated when sitting. Icing still helps with the swelling.
- Watch for warning signs (see FAQ below). But know that most of the time, things go exactly as expected.
The Truth Nobody Tells You
Recovering from a knee replacement tests you physically. It tests you emotionally too.
There will be a moment — usually around day two or three — when you think, "Why did I do this to myself? My old knee was better." Every knee replacement patient in history has had this thought. Every single one.
And then there will be a moment — usually around week three or four — when you bend your knee without thinking, or walk without a limp for the first time in years, and you will think, "This is the best decision I ever made."
The first week is the bridge between those two moments.
It is short. It is hard. And it is worth every day of it.
Questions Patients Ask Me Every Day
This is the most common question I get in Kannur, and it is a valid one. Our culture involves a lot of floor-level sitting. The honest answer: most patients with a knee replacement can sit on a low chair or a raised seat comfortably. Deep cross-legged sitting on the floor is generally not recommended because it puts extreme stress on the new joint and can reduce its lifespan. However, many patients gradually achieve enough bending to sit comfortably for prayer using a low stool or a raised platform. We will work on this together based on your progress.
Some pain and swelling in the first week is expected. It would be strange if there was none. Contact us immediately if you notice:
- Sudden severe pain that is getting worse instead of better
- The calf becoming very swollen, red, and painful to touch
- Fever above 101°F that does not come down
- Any fluid leaking from the wound that looks cloudy or has a bad smell
These are rare, but do not wait and watch. Call us.
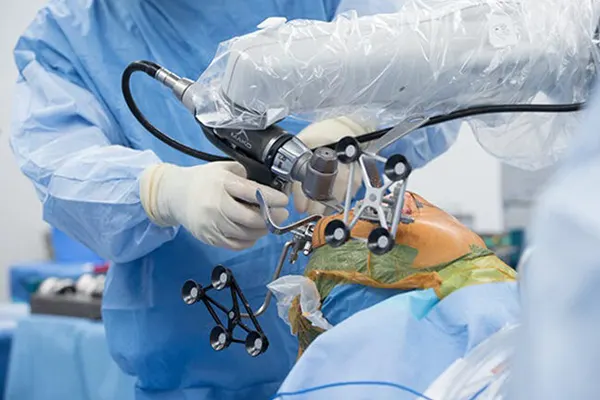
Because knee replacement recovery has changed enormously in the last ten years. The surgical techniques are more precise — we now use robotic-assisted technology at Aster MIMS that allows for a better-fitting, better-aligned joint. The pain management protocols are far superior. And the physiotherapy starts immediately. The old method of "rest for a month, then slowly start moving" actually produced worse results. Early movement is not being "too aggressive" — it is the global standard of care, and it is what I was trained to do at PGIMER Chandigarh.